Much of the most popular content in my portfolio is related to PTSD and trauma. I became interested in emerging research on trauma and PTSD while completing a trauma-focused Master’s degree in a Counseling Psychology Master’s program.
When I transitioned from research as a student to practice as a clinician, I remained interested in following the research on:
- Theories of understanding trauma,
- How trauma impacts us,
- What trauma recovery looks like, and
- What resources can help people who have experienced trauma thrive and experience post-traumatic growth.
This interest and educational background shapes many of the resources in my portfolio of downloads of educational mental health illustrations and resources.
Resources for Parenting Kids with Trauma
Being a parent to a child who has experienced trauma is an especially challenging job. Parenting is already incredibly difficult. When a child has experienced a traumatic event or series of traumatic events, the difficult challenges of parenting can be magnified.
Thankfully, many researchers are dedicated to finding the links between childhood trauma and resiliency, including Christina Bethell and her landmark research on identifying and promoting Positive Childhood Experiences. One challenge that many parents face when their child has experienced a traumatic event is knowing how best to support their child. While some parents believe not talking about the trauma event will best help a child to move on, other parents may pressure their child to talk about the experience in hopes that “processing” will help the child recover.
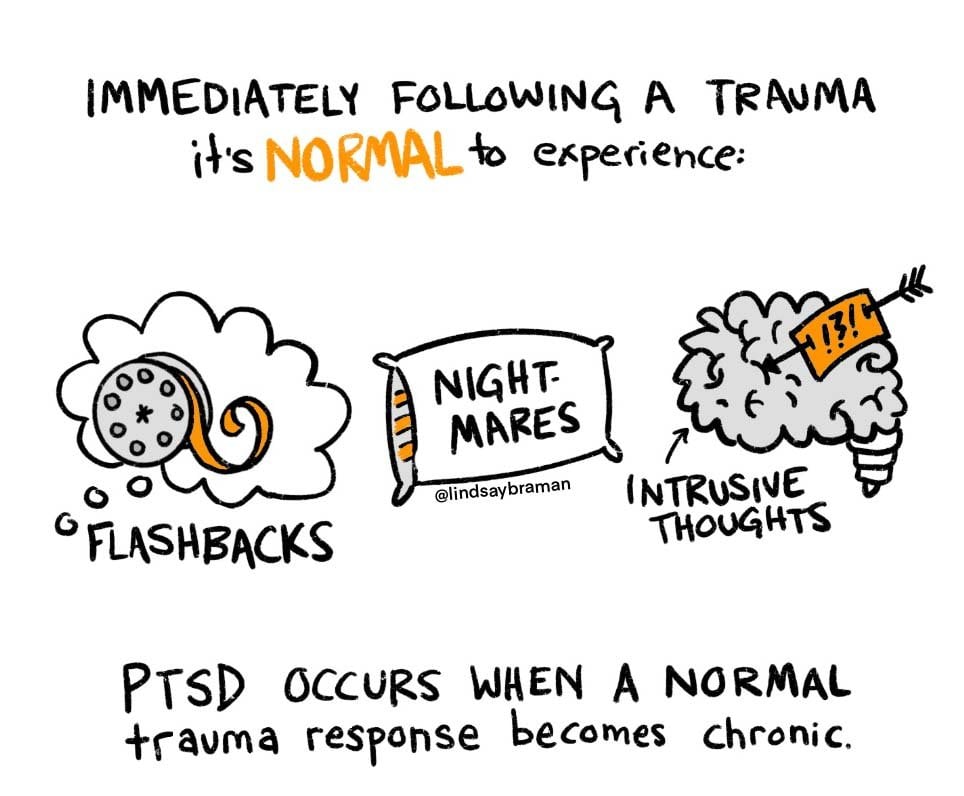
Interestingly, research indicates that a balance between these two perspectives may be the most effective in balancing care with resiliency. In fact, one large research study on children and traumatic experiences found that having nightmares, flashbacks, and intrusive thoughts immediately following the trauma wasn’t actually as accurate at predicting whether a child will develop PTSD as was what that child thought about their experience having nightmares, flashbacks, and intrusive thoughts. This research indicated that normalizing the brain’s work to integrate trauma (via “symptoms”) may correlate to a reduced likelihood for kids to have symptoms that qualified for a PTSD diagnosis at the six-month mark after the traumatic experience.
Much of supporting a child through – and beyond – a traumatic experience boils down to attachment and attuned caregiving. It’s about helping an individual child process in a way that is helpful for them. (Hint: it’s not the same way that adults process).
Supporting kids post-trauma includes:
- Providing support, without asking too many questions,
- Engaging with children through play – not conversations, and
- Accessing child-focused mental health professionals when appropriate.
Children with a strong attachment to an emotionally-healthy caregiver and a healthy (age-appropriate) capacity for emotional regulation may fare better following a traumatic experience than kids who don’t have access to these resources. While emotional regulation is a skill that we learn primarily through attachments with emotionally regulated adults, there are many teaching opportunities for helping kids develop the capacity to think and speak about their emotions. This can help them regulate their own emotions (which can lead to less acting out and a better ability to communicate their need for care in the future). For these kids, approachable resources like the mindful grounding deck and the kid’s feeling wheel can be helpful resources to help parents/caregivers and kids talk about feelings and help kids learn to describe what they are feeling.
Tools to Help Kids With Trauma to Self Soothe
It’s normal for kids who have experienced trauma to have a smaller capacity to regulate emotions (a smaller “window of tolerance”). In other words, they have a “short fuse” between feeling emotionally levelheaded and really upset.
It’s normal for all kids to have a window of tolerance that is smaller than mature adults with fully-developed brains. However, for kids who have experienced trauma, the window of tolerance can be tiny. This can explain how kids who have experienced trauma may be especially prone to moving from feeling good to a complete meltdown in a matter of moments. Kids in this state need support to help them calm down and often can benefit from tools to help them get grounded.
Getting “grounded” is a way of describing the feeling of being:
- Physically present to a body and
- Aware of our emotions.
Helping a child feel grounded is a far more effective way than discipline or even “time outs” to counter a child’s panicked and completely overwhelmed state.
Recognizing this in the kids I worked with (and even in myself!) in early 2020, I developed the mindful grounding card deck. This deck of 36 cards offers 34 ideas (plus an instruction card and a blank card for adding custom activities) that can help kids shift their focus onto one thing – like the weight of something in their hand or the color purple in a room – and, through that refocusing, help their brains return to a calmer state (i.e., their window of tolerance). The grounding card deck is designed to be used interactively as a game that empowers kids – while distracting them just a bit – with the invitation to pick a card and play the game, preferably alongside a parent.
Engaging Shared Family Trauma As A Way to Help Kids Heal
Increasingly, research is demonstrating that the best way to help children build resiliency to trauma is through doing our own emotional work and processing our own trauma as their adult caregivers. Parents and caregivers who are mindful of their own trauma, who demonstrate self-compassion, share appropriate disclosure about their own emotions, and who are emotionally attuned to their child (skills often learned, for parents who are themselves survivors of childhood trauma, through therapy) are better able to tune in, connect empathically and build resiliency to trauma in their own child.
One genre of psychological trauma that’s received more press in recent years is intergenerational trauma. Intergenerational trauma is passed down from parent to child, even if the child hasn’t experienced trauma directly. Often, this occurs through behavioral patterns, beliefs, or relational styles that a child unconsciously picks up from their parent(s). Research has determined that this is happening on a genetic level. The field of epigenetics studies how experiences we go through (such as a traumatic event, being parented by a traumatized parent, or – on the positive side – secure attachments to attuned parents, mentors, or caregivers) can turn off and on certain genes in our genetic makeup, resulting in changes to our health, brain function, and even appearance. Click here for a quiz on intergenerational trauma and more information.
Kids and COVID-19: Collective Trauma
There are few, if any, kids who have been totally spared from the psychological effects of the collective trauma we are all experiencing as fallout from the COVID-19 pandemic – or other similar experiences of collective trauma. Most kids, with the support of caring parents and teachers, will weather experiences like these with resiliency. However, if your child has a lot of very big worries about health, family, or safety – or if it seems like they’re having trouble processing through the experiences of the pandemic, it may be time to access resources to help your child deal with the very very big emotions and uncertainty we all feel as coronavirus affects people around the world.

While a check-in with a mental health professional may be appropriate for some kids, many kids who are working through collective stress within their community and family may find comfort and tools to process through face-to-face time, talking, playing, and creating about their concerns with a parent.
I’ve developed the COVID Kid’s Activity Book to help facilitate these types of parent-child processing. Appropriate for ages 3 to 11 (with age-appropriate levels of parent involvement), the COVID Kid’s Activity Book is a therapist-designed resource to help parents and children connect and to help kids understand the ways their families are helping them to stay safe and healthy through this difficult time.

Grounded in the research on Protective Childhood Experiences by Johns Hopkins University, the COVID Kid’s Activity Book is an evidence-backed resource to help kids understand how their families and communities are keeping them safe. In addition to other resources to support kid’s mental health, like the feelings forecast emotional regulation coloring pages and the COVID-19 Meaning-Making Family Activities I’ve curated, we can help our kids get through the collective trauma of COVID-19 and related experiences with less traumatic impact and more resiliency.
Resources for Parents and Kids Coping with Trauma:
- COVID Kid’s Activity Book
- Quarantine Well-Being Daily Check-In (appropriate for tweens and teens)
- Intrusive Thought Flow Chart and Worksheet (appropriate for tweens and teens)
- My Kid’s Version of a Feelings Wheel
Unique Self Care for Adult Survivors of Childhood Trauma
For people who’ve experienced childhood trauma and are now adults working towards better mental health, more satisfying relationships, and less intrusive trauma symptoms, this can be a journey that lasts a lifetime. Less often talked about, however, is that this recovery journey often results in post-traumatic growth. That is, people who experience trauma and engage deeply in recovery report more satisfying relationships and a higher level of empathy than if they had never experienced trauma in the first place.
A big part of recovery from trauma is learning self-care and self-advocacy. In my portfolio, I’ve created a number of resources for adult survivors of trauma to learn about how to access both of these things.
Things Trauma Survivors May Need
Meaningful art doesn’t have to be intricate, detailed, or perfect. That was the case with this messy doodle which, although simple, resonated with many and was widely shared on social networks after I originally posted it in early 2020. This illustration can serve as a gentle reminder to trauma survivors that it’s okay to need more care – or different care – than the people around us. Part of recovery is learning how to advocate for ourselves and what we need, and permission to do that can be a profoundly helpful boost on that journey toward asking for what we need.

How Good Therapy Works to Reduce the Impact of Trauma
Therapists- even trauma specialists- aren’t always great at explaining how trauma therapy works to reduce symptoms and improve the quality of life for trauma survivors.
It’s because much of effective trauma care takes place in the limbic brain (the “right side” of the brain that is feeling-focused, abstract, and emotion-driven). Because of this, it can be difficult to explain the processes by which therapy can help trauma survivors recover. One of the best models for trauma recovery is the one I’ve illustrated based on a 1994 description in the book Naming the Shadows. In it, Susan Roth and Ronald Batson describe a model in which the impact of trauma takes up lots of space within a “self.” With good therapy, the impact of trauma shrinks. In my model, taking up less and less space within a “self” allows for more and more positive emotions and relationships to inhabit and flourish in that space.
Disclosing Trauma in Relationships
For many trauma survivors, there’s a deep desire for the people they care about to know about their trauma, paired with a deep fear that disclosing their trauma narrative will result in the other person responding poorly, distancing, or “ghosting.” Sometimes, how trauma survivors tell a trauma narrative can make this fear sphere a self-fulfilling prophecy.
Letting Intimacy Grow to Support Disclosure
In hopes of relieving the anxiety of telling, not telling, and fearing consequences, many trauma survivors may share their trauma in a way that may backfire. Relationships need time to mature and develop the necessary trust and intimacy to hold difficult topics well. Sometimes, we may overshare too quickly, in a way that doesn’t honor ourselves or a partner, creating a dynamic that results in feeling alienated or misunderstood.
One way that some trauma survivors are able to navigate this is through what I call “tiered disclosure.” Tiered disclosure is like a wedding cake: each layer is a little bigger than the one before it. It’s possible to disclose trauma similarly, sharing a little bit at a time to give ourselves a chance to test and see how a little bit felt before sharing more. This also gives our partners the opportunity to be thoughtful and ready to hear more, rather than putting them in a position where they are expected to provide care and empathy while processing the shock of hearing that something awful has happened to someone they care about.
Handling Intrusive Thoughts – Flowchart
Intrusive thoughts are one of the most common markers of trauma that adult survivors of childhood trauma experience. Although alarming and upsetting, skills for handling intrusive thoughts well can be learned. Learning to expect intrusive thoughts and preparing in advance for how to deal well with them can equip us to receive them and put them immediately to rest instead of letting them interrupt and upset us.
Fight, Flight, Freeze, Fawn
The “polyvagal theory” is a fancy term that describes the concept behind the Window of Tolerance. The polyvagal theory encompasses responses beyond just shutting down, blowing up, being somewhere in the middle, or being “okay” (as shown in the Rainbow of Emotional Regulation). It also includes categories for two additional responses: “fawn” and “freeze.” Understanding the full range of responses in the Fight, Flight, Freeze, Fawn model can help us understand our own responses, be more compassionate, and respond with even better self-care.

Additional Resources for Adult Survivors of Childhood Trauma:
Trauma in the Classroom
Although teachers were never intended to be mental health professionals, understanding and responding well to various mental health concerns is an increasingly important skill in the classroom. In this section, I have collected some of my resources for teachers on the topic of trauma, trauma-informed teaching, and providing mental health / emotional regulation education in classroom content.
Trauma Triggers in the Classroom
What are triggers? Should class content include trigger warnings?
Triggers are different for every individual. What often gets confused (as pop culture adopts more and more psychology-based language) is what triggers actually are and what they aren’t. Despite a changing use of language that has adapted “trigger” as a synonym for “upsetting” – when it has traditionally been used to refer to trauma triggers – there’s a BIG difference between something that is simply upsetting and something that is a trauma trigger.
Trauma Triggers are: Trauma triggers take us out of our body. They usually come by surprise and cause dissociation from time, relationships/conversations, and our body sensations. Trauma survivors may or may not be aware when they are triggered. Growing awareness of what our triggers are, how they affect us, and the care we need when triggered is a huge part of the recovery process for trauma survivors. The trigger tracking worksheet can help develop awareness and skills for self-advocacy, as individuals identify triggers so that, with appropriate support, they can engage and process triggers rather than allowing triggers to grow stronger through total avoidance.
Trauma Triggers are not: Difficult information is not a trigger. Feeling upset, angry, defensive, or other feelings is normal and healthy when we hear difficult information. Getting upset when we hear or are exposed to upsetting things is not a trigger. Getting upset, in this context, is not directly related to a mental health condition. It’s part of how a healthy brain processes negative information. This doodle series on trauma triggers vs. just uncomfortable topics explores this concept through visuals, Venn diagrams, and a simple side-by-side comparison.

Trigger Warnings in Classrooms:
Do trigger warnings work when trauma triggers are at play? The evidence seems to suggest they do not. A recent research study on whether trigger warnings are helpful was conducted at Harvard University. Researchers found that trigger warnings for most people reporting a traumatic history raised anticipatory anxiety significantly and only moderately decreased exposure anxiety. Simultaneously, trigger warnings increased perceptions in the non-traumatized population that people who had experienced trauma were more fragile. This belief could lead to a lowered capacity for resilience to trauma for those who might have experienced a traumatic event in the past. These findings were in line with other research studies on the topic.
How to Language Trauma to Support Recovery
Supporting trauma survivors in the classroom should be a collaborative effort. When teachers, caregivers, and mental health professionals work collaboratively, children and teens can have recovery and thriving post-trauma.e of
In addition to supporting positive childhood experiences (a new scale that’s the opposite of ACEs), one easy change we can make is to intentionally choose language and ways of framing our conversations on trauma in ways that support resiliency. One of the ways we can support this in the classroom is by supporting experiences for resiliency in kids. Learn more in my article on how to talk about trauma in a way that promotes resiliency.
Trauma-Informed Classroom Grounding Kit
You’re probably familiar with elementary and preschool classrooms that include a “calm down” space filled with sensory items and other resources for helping kids get settled and grounded when they are upset. Although it looks different, this support can continue in the classroom into junior high and high school.
One way we can support older kids and teens who have experienced trauma is by providing resources to support a good range of emotional regulation. A basic trauma-informed classroom kit that includes a deck of grounding activities can be a way to provide access in our classrooms for kids and teens who have experienced trauma to use to get grounded.
Additional Trauma-Informed Resources for Teachers and Classrooms:
Resources for Therapists and Mental Health Professionals Teaching about Trauma, PTSD, and Trauma Recovery
Most of our work to help individuals recover from trauma involves empathic work, building an alliance, and applying appropriate interventions. Psychoeducational interventions are also effective tools for trauma survivors. Trauma survivors often feel confused by their own responses. Because of this, many report a positive benefit simply through understanding that other trauma survivors share their experiences and that there are evidence-based resources that can help them grow the skills needed to support their recovery.
Avocado Model for Teaching Trauma Recovery
Understanding trauma and how it impacts the brain can be a huge help in recovery. As outlined in the Trauma vs. Normal Post-Traumatic Responses research-article sketchnote, how we frame our response to trauma seems to impact how well we cope with what we have experienced.
This avocado image is how I teach about trauma and how trauma impacts us. Because it’s non-pathologizing and friendly (and cute!), it’s memorable and easy to understand. This makes it easier for trauma survivors to share with friends and family and ultimately helps them develop better self-advocacy and social support. The trauma avocado model is perfect for clinical, classroom, and personal use. It’s an easy-to-understand visual for children and adults that explains trauma and how it impacts us without being overly clinical. A fun, handwritten style font and the familiar imagery of an avocado make this psychoeducational illustration approachable and easy to use.
Additional Professional / Psychoeducational Resources for Mental Health Professionals Treating Trauma:

